Comprehensive Guide to Clinical Pathology Concepts
Clinical Pathology
Purpose
The Concept Explainer Sheet is designed to:
- Simplify complex pathology theories into workplace-relevant explanations.
- Use realistic examples and visuals to demonstrate how laboratory tests relate to patient diagnosis.
- Show learners how to apply theoretical knowledge in practical lab scenarios.
- Highlight UK regulations and best practices in laboratory safety, sample handling, and professional conduct.
Section 1 – Principles of Pathology
Definition:
Pathology is the study of disease, including its causes (etiology), development (pathogenesis), and effects on the body.
Key Concepts:
| Concept | Explanation | Workplace Example | Visual/Diagram |
| Disease Etiology | Cause of disease (infection, genetics, environmental) | Identifying bacterial cause of urinary tract infection | Diagram showing bacteria in urinary tract |
| Pathogenesis | How disease develops | RBC destruction in haemolyticanaemia | Flowchart showing RBC lysis → anaemia → fatigue |
| Lesion | Structural/functional abnormality | Skin biopsy showing malignant cells | Cross-section image of tissue lesion |
| Clinical Manifestation | Symptoms/signs | Jaundice from liver dysfunction | Diagram of liver → bilirubin buildup → yellowing skin |
Application in Diagnostics:
- Lab tests measure biological markers reflecting these pathological processes.
- Example: ALT/AST tests for liver damage, CBC for anaemia detection.
Section 2 – Common Diseases and Laboratory Detection
Blood Tests (Haematology)
| Disease | Test | Normal Range | Abnormal Indicator | Visual Aid |
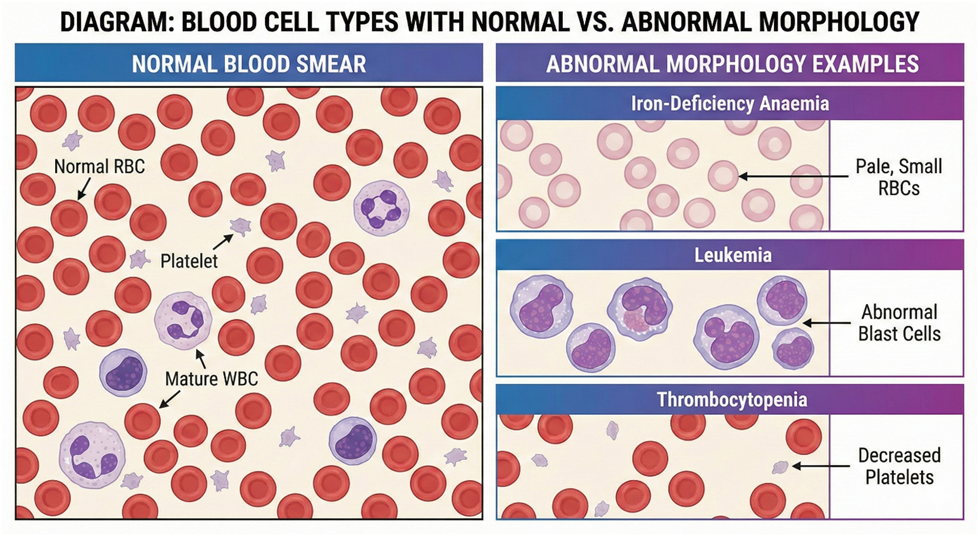
| Iron-deficiency anaemia | Hemoglobin, Hematocrit, MCV | Hb: 13.5–17.5 g/dL | Low Hb & microcytic RBC | RBC diagram with pale cells |
| Leukemia | WBC count, differential | 4–11 x10⁹/L | High WBC, abnormal blast cells | Microscopic image of blast cells |
| Thrombocytopenia | Platelet count | 150–400 x10⁹/L | Low platelet count → bleeding risk | Diagram of low platelets in blood smear |
Urine Tests (Clinical Biochemistry)
| Condition | Test | Indicator | Workplace Example |
| Diabetes Mellitus | Urine glucose & ketones | +1 to +3 indicates hyperglycemia | Midstream urine collected, tested using dipstick |
| Urinary tract infection | Urine culture | Presence of bacteria | Sterile container, incubated for 24h |
Tissue Tests (Histopathology)
- Purpose: Detect structural changes in tissue.
- Example: Biopsy showing squamous cell carcinoma.
- Visuals: Histological slides highlighting abnormal cell growth.
Section 3 – Role of Samples in Clinical Investigations
Blood Samples:
- Assess haematology, biochemistry, immunology.
- Tube types: EDTA (hematology), serum (biochemistry).
- UK Guidance: Use PPE, proper labelling, and follow Health and Safety Executive (HSE) blood handling standards.
Urine Samples:
- Detect metabolic or infectious conditions.
- Collected as midstream, first-morning samples.
- Stored at 4°C if not immediately analyzed.
Tissue Samples:
- Examine cellular morphology to confirm disease.
- Fixation in formalin, then processed for histology.
- Safety: Follow COSHH (Control of Substances Hazardous to Health) regulations.
Visual Example:
Flowchart: Patient → Sample Collection → Lab Analysis → Results → Diagnosis
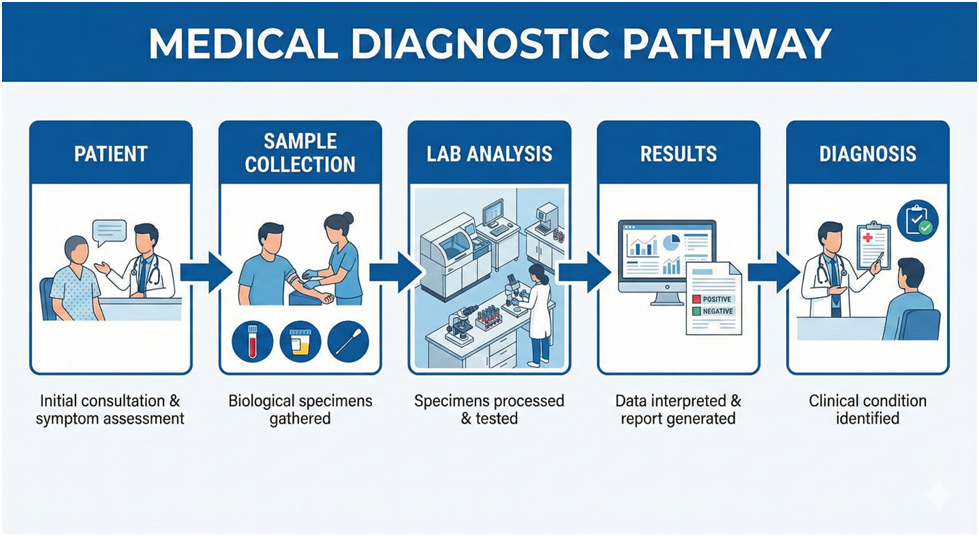
Section 4 – Linking Lab Results to Clinical Symptoms
| Symptom | Lab Test | Expected Findings | Interpretation |
| Fatigue, pallor | CBC | Low Hb/Hematocrit | Iron-deficiency anaemia |
| Jaundice | Liver function tests | High bilirubin | Liver dysfunction or hemolysis |
| Frequent urination | Urine glucose | High glucose | Possible diabetes mellitus |
| Abnormal lesion | Biopsy | Malignant cells | Cancer diagnosis |
Visual Aids:
- Diagrams connecting symptom → abnormal lab value → disease.
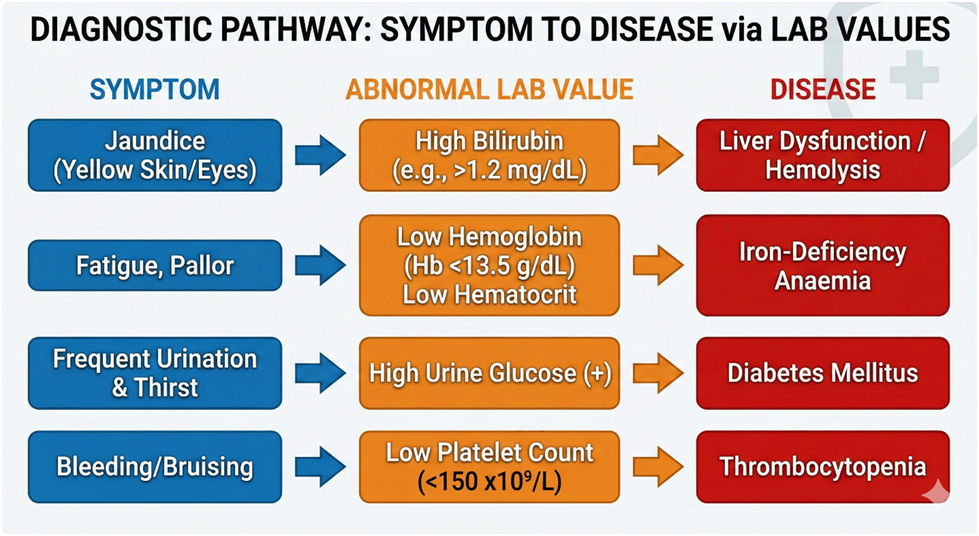
- Colour-coded tables highlighting normal vs abnormal ranges
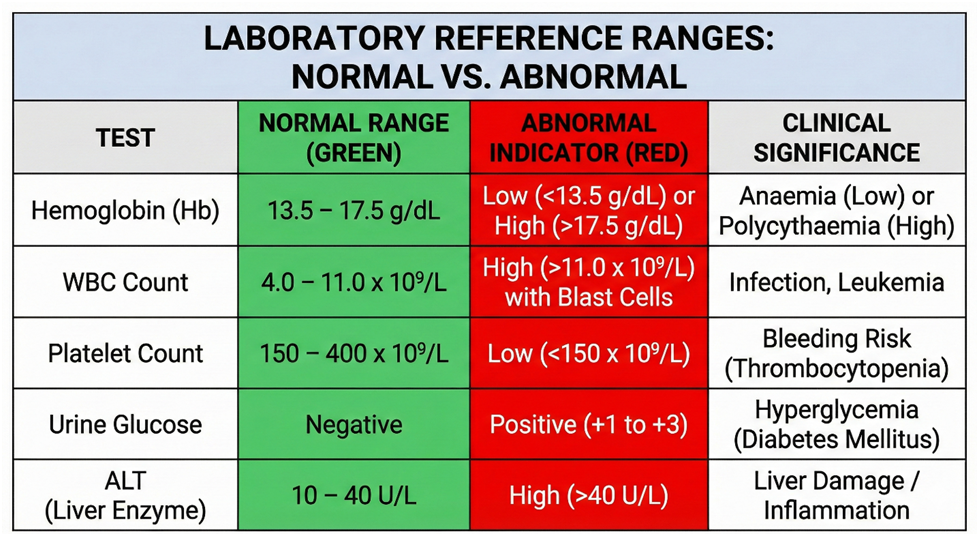
Section 5 – Recognising Abnormal Values and Significance
Step 1: Identify deviations from reference ranges
Step 2: Assess clinical relevance
Step 3: Report under supervision
Example:
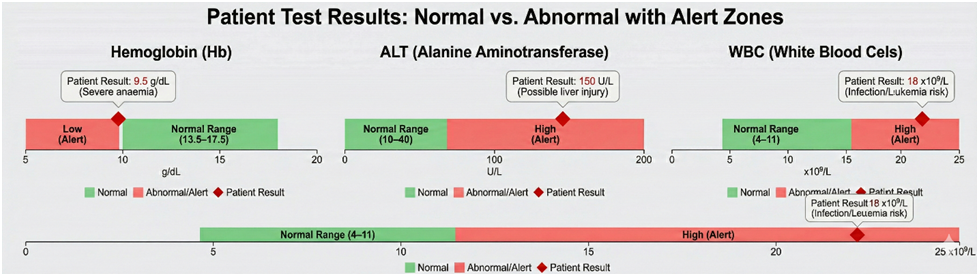
| Test | Result | Reference | Significance |
| Hemoglobin | 9.5 g/dL | 13.5–17.5 | Severe anaemia; requires intervention |
| ALT | 150 U/L | 10–40 | Possible liver injury or hepatitis |
| WBC | 18 x10⁹/L | 4–11 | Infection or possible leukemia |
Visual Aid:
Graphs showing normal vs abnormal results with alert zones.
Section 6 – Best Practices and Safety Compliance
UK Regulatory References:
- Health and Safety at Work Act 1974 – safe laboratory environment.
- Control of Substances Hazardous to Health (COSHH) Regulations 2002 – chemical handling.
- UK Good Laboratory Practice (GLP) – sample traceability and documentation.
- NHS Confidentiality Guidelines – patient data protection.
Practical Tips:
- Always label and store samples correctly.
- Wear PPE (gloves, lab coat, eye protection).
- Report abnormal results promptly to supervising staff.
- Ensure accurate and legible documentation.
Learner Task Section
Required Evidence:
Technical report or explainer on the use of laboratory instruments and basic automation in pathology; and a maintenance and calibration log template for a pathology instrument.
Objective:
Demonstrate technical understanding of how automated pathology platforms (e.g., Chemistry or Haematology analyzers) support diagnostic precision. You must show how the “Standard Operating Procedures (SOPs)” and “Calibration Cycles” discussed in this sheet are applied to specific pathology equipment to ensure the accuracy of disease indicators.
Instructions:
Pathology Instrumentation Explainer:
- Select one major piece of automated pathology equipment (e.g., a Clinical Chemistry Analyzer for liver function tests or a Tissue Processor for histology).
- Explain the scientific principle behind the instrument’s operation (e.g., Photometry, Ion Selective Electrode, or Histological Processing cycles).
- Discuss how automation reduces “Inter-operator Variability” compared to manual pathological methods.
Maintenance and Calibration Logic:
- Develop a “Maintenance and Calibration Log Template” for your chosen pathology instrument.
- Detail the requirements for Daily Start-up, Weekly Cleaning, and Calibration Verification (checking the instrument against known standards).
- Explain why a “Calibration Drift” could lead to a false pathological diagnosis (e.g., over-reporting blood glucose levels).
Troubleshooting & Regulatory Compliance:
- Describe the corrective actions required if an instrument fails its “Internal Quality Control (IQC)” during a pathology run.
- Identify the specific SOP and UK regulation (e.g., MHRA Guidance for IVD devices) that governs the handling of faulty diagnostic equipment.
Integration of Pathology Workflow:
- Create a flow chart showing how the instrument integrates into the pathology workflow: from Sample Loading and Barcode Scanning to the transmission of results to the Laboratory Information Management System (LIMS).
Professional Rationale:
- Write a 500-word justification explaining why a technician must still possess manual skills (e.g., dilutions or slide staining) despite the prevalence of high-throughput automation in modern pathology labs.
